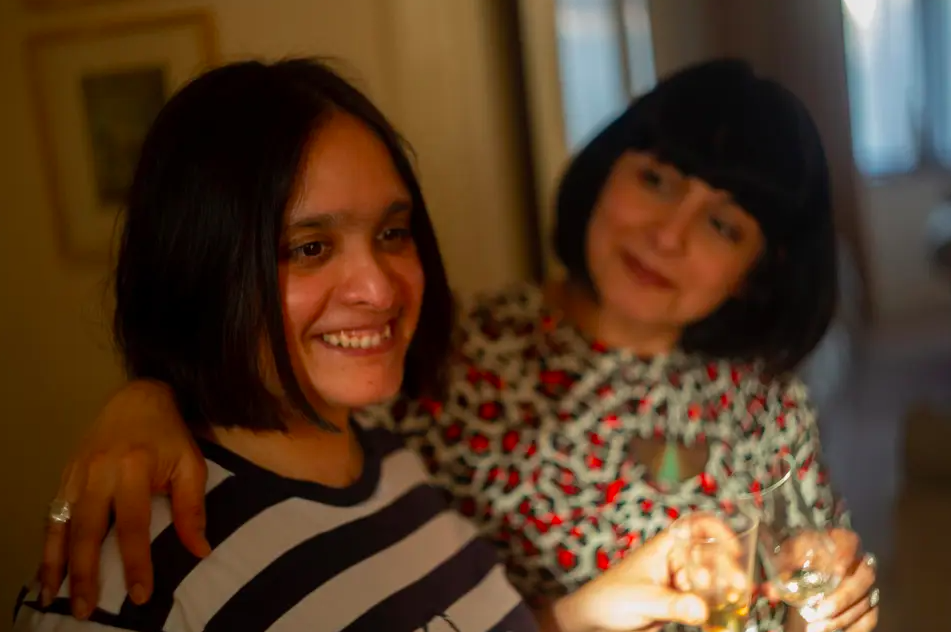I wrote a personal piece for the Guardian about how Covid-19 is impacting disabled people and families.
Coronavirus has thrust us all into a new normal. Life has come to feel the same yet different. However, for some communities Covid has undermined their very ethos.
My youngest sister Raana, who has a learning disability, has lived in a supported living community in Hampshire for 10 years. We chose the charity that runs her home for its values. It creates a sense of belonging and purpose, focuses on abilities and is governed by the belief that everyone has the right to be involved in society.
Covid-19 means that not only are the guiding principles of the charity are at risk, but my sister’s independence is being undermined.
You can read the piece on the Guardian website here.